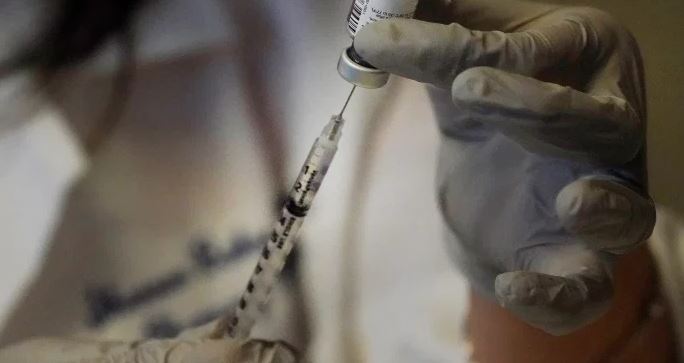
All LTC residents, staff in Toronto, Peel, York and Windsor-Essex set to receive COVID-19 vaccine by Jan. 21
COVID-19 vaccines are expected to be in the arms of long-term care residents in Toronto, Peel, York and Windsor-Essex by Jan. 21, according to the Ontario government.
The province’s COVID-19 Vaccination Task Force provided an update on the Pfizer BioNTech and Moderna vaccine rollout plan Tuesday morning.
Health officials say the goal is to inoculate all long-term care home residents, staff and caregivers in those hot spots, within the first three weeks of the New Year.
The government did not provide a specific number of how many residents and staff this would include but retired General Rick Hillier, who is leading the province’s vaccine task force, later told a pool camera that it will take about 55,000 doses of the vaccine.
Approximately 53,000 doses of the Moderna vaccine arrived in the province during the week of Dec. 28 and Hillier said that about 56,000 more doses of the Moderna vaccine are expected to arrive in the province by tonight or tomorrow. That supply, he said, will be fully exhausted by next weekend.
Nearly 3,000 doses of the vaccine have been administered by Jan. 3 and 1,000 more doses are expected to be handed out to a total of 26 long-term care homes between Jan. 4 and 6.
Each of the two Moderna vaccine doses must be injected 28 days apart.
“We are working around the clock to get these vaccines into peoples’arms. As a matter of fact as we ramp up, as you might have noticed throughout this pandemic, it might take us a couple weeks to ramp up but once we get the machine going in Ontario we kick but anywhere in the country or North America,” Premier Doug Ford said during a photo-op at Queen’s Park on Tuesday afternoon. “No matter whether it is the testing, the PPE or any other challenge we have had once we put team Ontario behind it we become the leaders and we will become the leaders in North America America once this machine rolls out.
As the province focuses on vaccinating the most vulnerable in the hardest-hit regions first, doses of the Moderna vaccine is expected to be expanded to three more Public Health Units (PHU) by next week.
The government did not say which additional PHUs will be included in this rollout.
The government also says that they are “developing protocols to safely move the Pfizer-BioNTech vaccine beyond the point of delivery,” thus allowing them to take that vaccine into long-term care homes as well.
University of Toronto professor and epidemiologist Colin Furness said vaccinating all long-term care residents in those hot spots will be a milestone but the goal might be offset by the spike in COVID-19 cases.
“We are getting over 3,000 cases a day in Ontario. If even a tiny number of those are fatal, which they are, what we might see will be an increase in mortality. However, I am sure everyone wants to see long-term care homes taken out of the equation. We all want to see the residents safe and the staff who work there as well,” Furness told CP24.
The province logged 3,128 new COVID-19 cases on Tuesday, nearing the record-high of 3,363 cases reported on Saturday.
NDP leader Andrea Horwath said the government dropped the ball with their vaccine rollout plan.
"We don't have time for bumps in the road. The government should have planned for this vaccine rollout far earlier than they did. I can tell you that if we were in this situation, we certainly would have ramped up our protection of seniors in long-term care in the first place over the summer," she said during a virtual conference with the media on Tuesday.
Meanwhile, the first COVID-19 vaccinations are scheduled to be administered to First Nations communities this week.
Long-term care and chronic care residents in Sioux Lookout and along the Coastal communities are expected to start receiving the vaccines sometime this week.
The government said a plan is underway to begin vaccinations in fly-in First Nations communities in the north.
The government also released a "risk matrix" which will be used to determine vaccine prioritization among health-care workers. The guideline weighs the risk of exposure among patients and within a healthcare setting. It also considers the criticality of a health-care worker's role and if they cannot work remotely or work in areas with limited capacity.