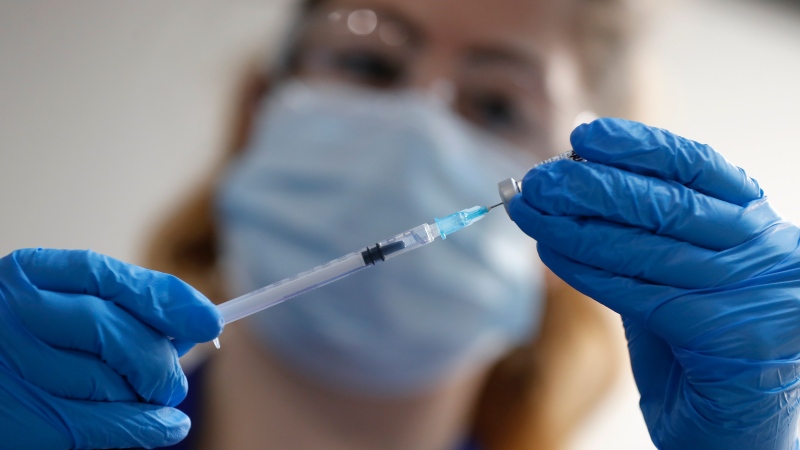
Pilot program aims to improve trauma-informed care to LGBTQ+ people
TORONTO -- A team of researchers at the University of Toronto’s Dalla Lana School of Public Health have launched a pilot program aimed at improving health providers’ ability to give trauma-informed care to LGBTQ+ people.
Over the last decade, studies have shown that LGBTQ+ people have trouble accessing health and social services. Transgender and non-binary people in particular experience significant health-care barriers, according to a recent report published by Trans Pulse.
Researchers say that a lack of LGBTQ+ cultural competency on the part of health-care providers, and the organizations they work within, have hindered their ability to give patients the care they need.
“There are unique forms of trauma that members of the 2SLGBTQ+ community experience, as well as unique challenges in accessing care,” Michelle Tam, project co-ordinator and PhD student at the Dalla Lana School of Public Health, said in a statement.
Tam and her team are attempting to address this issue through a series of virtual workshops on trauma-informed care and LGBTQ+ competency, with financial support from the Public Health Agency of Canada.
The six-module program was taught in-person across Ontario in cities like Ottawa, Toronto, Thunder Bay, London and Timmins. However, the workshop switched to an online format in June to comply with COVID-19 restrictions.
The training is designed for providers working in health care, mental health and other social services. Researchers hope the workshop will help prevent stigmatization or the re-traumatization of LGBTQ+ people who access support.
The team defines trauma-informed care as an approach by health providers to “recognize the far-reaching impacts of trauma on individuals and the ways in which service providers and organizations may unintentionally perpetuate trauma.”
“As a result of these experiences of discrimination, many 2SLGBTQ+ people choose not to access care when they need it, which means that their underlying concerns may never be addressed, and the problems that result from those concerns (such as depression, anxiety, or drug use) may worsen,” the program’s principal investigator Lori Ross said in a statement. “This likely contributes to the ongoing health disparities we see in Canada (and elsewhere) associated with sexual orientation and gender identity.”
She added, “Better equipping service providers to meet the specific needs of 2SLGBTQ+ people, particularly as those needs relate to experiences of trauma, will help to address these disparities and lead to better health and well-being for 2SLGBTQ+ communities.”
A 2010 study published in the American Journal of Public Health found that LGBTQ+ people are more likely to experience PTSD and violence beginning in their childhood.
The study noted there is “an urgent need for public health interventions aimed at preventing violence against individuals with minority sexual orientations and providing follow-up care to cope with the sequelae of violent victimization.”
So far, Tam says the workshop has reached about 300 service providers across Ontario and 116 unique organizations, services and institutions.
Although there are other initiatives to train service providers on trauma-informed care and LGBTQ+ competency separately, this is one of the first programs specifically designed to focus on the two issues jointly.
While researchers say there is a significant need for the development of a national initiative, Tam and her team are currently in the process of evaluating the pilot stage of the program and hope to explore opportunities to deliver the workshops across Canada in the future.